Over the two-year course of this COVID-19 pandemic, I have taken extra steps to keep myself and my family safe. I’ve kept abreast of the latest medical advice and research. I’ve invested in N95 and KN95 masks. I’ve hauled around my HEPA air filter to places where proper ventilation would be hard to come by. Most importantly, whenever I’ve had the slightest concern that any health symptoms I’d been experiencing might have been COVID, I have gotten tested with Wake County’s free PCR COVID tests. Six times I’ve done this, and six times I received a relieving result of negative. Most recently, we were shipped a set of four COVID antigen tests free from the government, and a test using one of those turned up negative, too.
I kept my precautions up, thinking I had succeeded in avoiding an COVID infection. It turns out I may have been wrong and didn’t even know it.
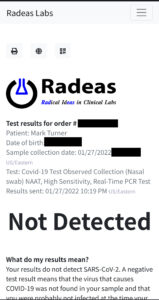
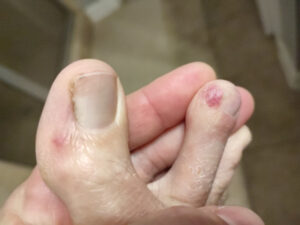
Last week, I noticed that one of my right toes was a little stingy and looked bruised. I didn’t recall injuring it so I wondered if it might be the “COVID toes” I’d heard about. See, COVID patients reported sores on their toes (mainly. Fingers may be involved, too), and my toe looked suspiciously like this. COVID attacks the vascular system in addition to everything else it hits, and red toes can be a symptom. Around that time, I had an attack of my Reynaud’s Syndrome, with some of my fingers turning numb and white for over an hour. This red toe effect could also be caused by Reynaud’s (which is also a vascular disease), so I couldn’t say for sure what was what. Thus, I popped open the antigen test and 15 minutes later it told me I was COVID negative. Sure, an antigen test is not as accurate as a PCR test but this was at the height of my symptoms so I assumed if I was going to pop positive on anything it would be right at that moment. But, no, it was negative!
Over the weekend, I got to thinking about how my body reacted to the primary, secondary, and booster COVID vaccines I had gotten. Basically, I didn’t react at all! There were no noticeable side-effects whatsoever. I was thinking about this and deciding that perhaps my reaction to the actual virus would be a similar non-event. I decided to contact the VA to schedule a COVID antibody test, knowing that this might show whether I’d been exposed and didn’t know it.
Continue reading